Shelagh Fogarty 1pm - 4pm
11 October 2021, 10:58 | Updated: 12 October 2021, 07:35
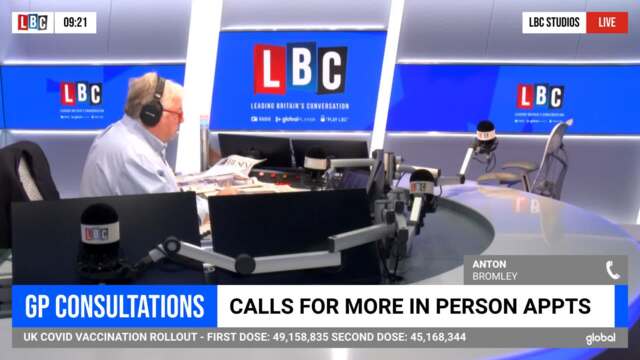
Caller breaks down explaining how his wife died
A man whose wife died of cancer aged just 44 says she "would have been saved or treated much earlier" if her GP had paid a home visit.
Anton has been left to raise three children aged 15, 14 and 9 - the oldest of whom is disabled - alone following the death of his wife three months ago.
He told LBC's Nick Ferrari that when she developed "very serious pain" he "begged" the GP "to pay a home visit and to advise me to take her to the cancer unit straight away or not".
READ MORE: GP shortage in poorer areas sparks concerns over widening health inequalities
Instead, the GP sent a rapid service nurse who carried out some basic tests.
It comes as it was revealed that the average GP is now working a three-day week, with a drop in working hours particularly "significant" in the years since 2017.
Anton continued: "When she collapsed I took her to A&E and eventually to the cancer unit, her cancer had spread to the brain."
He described holding his wife's hand in the hospital and coming to terms with the fact it was too late for her to be saved.

'Devastated' caller’s life is on line as cancer treatment cancelled
He said: "The statistics show 10 million online consultations, those are utterly rubbish, it's not effective, there's no point getting a consultation, it should be an effective consultation.
"My wife would have been saved or treated much earlier if that doctor would have paid a home visit."
Anton, from Bromley in south-east London, added that he checked on the NHS England website and was "clearly" entitled to a home visit.
He said: "The doctors are supposed to make home visits for the people who can't come to the surgery but it's not happening."
READ MORE: Gritter driver shortage could lead to icy roads this winter
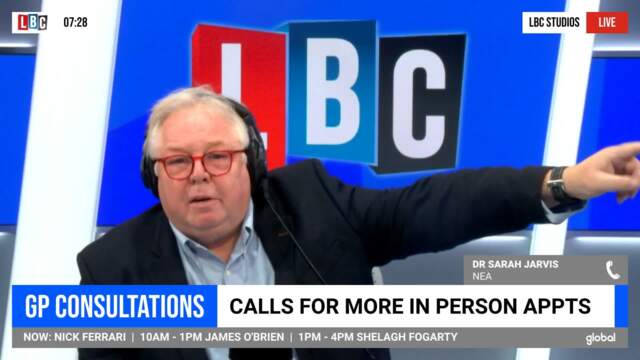
Nick Ferrari clashes with GP over part-time doctors
The devastating call comes amid fears patients in England are facing a "postcode lottery" over seeing a GP in-person, with the worst-affected areas served by half the number of doctors as the best.
There is on average one GP per 2,038 people across the country, a 5% rise since 2015, new analysis has shown.
However, despite this rise there are also huge disparities across England.
Some areas have seen an increase of around 40% in people per GP over the same period.
For example, Hull now has one GP for every 2,821 people, more than double the 1,279 people per GP in Wirral.
The Liberal Democrats, who commissioned the analysis, have called on the Government to train more GPs to ease the "postcode lottery".
The Daily Telegraph reported that, according to research commissioned by the Department of Health, GPs carried out just 6.6 half-day sessions a week - the equivalent of just over three days - in 2019.
This is said to be the lowest on record and down from 7.5 sessions in 2010.
The National GP Worklife Survey of 1,332 GPs, carried out by the University of Manchester, also showed just 59 per cent of GPs' time was spent on "direct patient care" in 2019, down from 63.1 percent in 2010.
Although the research is from before Covid it comes amid increasing concerns over access to face-to-face appointments which have arisen during the pandemic.
However, a number of GPs have hit out at the continued criticism over a fall in such appointments, and have called for more support from the Government.
Professor Martin Marshall, chair of the Royal College of GPs, said practice doctors are "stretched beyond endurance" and the pressure is "taking its toll on the mental health and wellbeing" of his teams.
He explained that GPs are delivering care to a growing number of patients with increasingly complex health conditions, "under intense workload and workforce pressures that have only been exacerbated by the pandemic".
"Whilst workload escalates, between September 2015 and March 2021 the numbers of full-time equivalent GPs dropped by 4.5%," he said.
"This is despite the Government's commitment to bolster the workforce with an additional 6,000 GPs by 2024.
"Heavy workloads are taking their toll on the mental health and wellbeing of our teams. A recent RCGP survey showed 60% of GPs that responded reported that their mental health has deteriorated over the last year - with a third saying they feel like they can't cope at work at least once a week.
"As a result, GPs are burning out and many are feeling forced to leave the profession earlier than they planned.
"In some cases, practices are closing completely. Figures show nearly 100 closed in 2020, and whilst some will be due to surgeries merging, some will be because vacancies can’t be filled or the pressure has simply become too much."
READ MORE: 'We don't have enough desks': Health Sec admits just 30% of staff are back in the office

GP sets out shocking scale of abuse doctors are facing
Responding to reports that the "average GP is now working a three-day week", Dr Richard Vautrey, British Medical Association GP committee chair, said the very notion of a 'part-time' GP is "often anything but".
He defended the profession against continued criticism over a fall in in-person appointments.
"The data used in this [Daily Telegraph] article actually shows that the average hours worked by a GP in England is around 40 hours per week – the same as most full-time jobs," he said.
"To focus purely on 'sessions' is an incredibly crude measure. Each morning or afternoon 'session' of work for a GP is defined as 4 hours and 10 minutes long. In reality, the sheer scale of workload means that both a morning session and an afternoon session often extend well beyond this, which means many GPs in reality work 10 to 12-hour days.
"When even 'part-time' GPs are working at such a pace, it's clear to see that current levels of workload – made worse by piles of admin and bureaucracy - are not sustainable. By removing some of this unnecessary bureaucracy, GPs would be able to devote more of their working hours to seeing patients who need them.
"GPs who work fewer sessions or hours in practices may well be dedicating time elsewhere in the NHS and wider health system – for example training younger doctors and medical students, working in hospitals or conducting research to ensure better healthcare in the future.
"We should also get away from the idea that working flexibly in itself is a bad thing. There are more women than men working as GPs today, and the fact that general practice offers flexibility that allows people of all backgrounds to balance their GP work with other commitments, such as family and caring responsibilities, should be celebrated and not condemned. Without embracing this, we risk losing these talented clinicians all together and therefore making access and workload problems a lot worse."