Ben Kentish 10pm - 1am
15 February 2022, 19:04
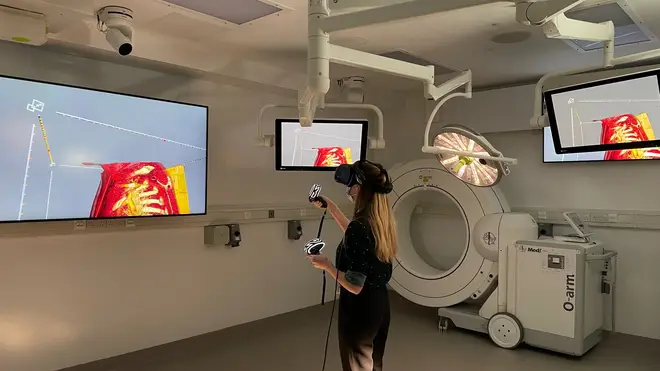
Researchers hope using VR to plan and practise procedures will shorten operating times and reduce the need for multiple surgeries.
New virtual reality (VR) technology could improve outcomes for the thousands of patients who undergo surgery for heart defects present from birth.
Every day in the UK around 13 babies are diagnosed with congenital heart disease – heart conditions that develop in the womb, before a baby is born.
Depending on how severe the condition is, they may need multiple surgical or keyhole procedures to help their hearts function normally.
Researchers hope using VR to plan and practise procedures will shorten operating times and reduce the need for multiple surgeries, leading to better outcomes and experiences for patients and their families.
It is hoped the technology could be in regular use within the next two years.
The method uses a number of scans that are routinely used to plan surgery to create a three-dimensional, beating digital double of the heart.
While these scans are regularly used to help plan surgeries, they are usually only viewed on a flat screen.
But using the VR technology, surgeons are immersed into the heart, allowing them to interact with and manipulate the images however they like.
They can also test options for the procedure in VR before they get to the operating table.
Darren and Gemma Nesbitt have a daughter, Rosie, with congenital heart disease.
At just 10 days old she underwent open heart surgery at Evelina London Children’s Hospital to repair problems with some of her heart’s major blood vessels.
Mrs Nesbitt said: “You’re given so many different pieces of information when your child is diagnosed with a heart condition, but I really struggled to understand what the problems in Rosie’s heart meant for her.
“Being able to see her heart using this technology would have been a huge help for me to understand more about her complex heart structure.”
Rosie, now 10, had a further procedure at the age of nine to close a hole in the wall between her ventricles and repair a valve in her heart.
Mrs Nesbitt added: “Anything that can give surgeons more confidence going into an operation, or that could shorten the time spent operating, would be a major help.”
Mr Nesbitt said: “This technology could bring real comfort and reassurance to families like ours.”
When asked how she felt about seeing her heart using the technology, Rosie said: “It would be so cool.”
Lead researcher John Simpson, professor of paediatric and fetal cardiology at Evelina London and King’s College London, said: “Procedures to repair the heart’s anatomy can be complex, and surgeons don’t like surprises.
“Our technology will allow surgeons to plan and practise these procedures, and we’re currently applying for approval for it to be used in this way.
“We think that this technology could also be used outside of congenital heart disease surgeries, to plan any procedure which aims to repair a structural problem within the heart, such as valve surgery in an adult patient.”
The technology, funded by the British Heart Foundation (BHF), has been developed by researchers at Evelina London Children’s Hospital and King’s College London.
Trials of an early version of the technology, which only used ultrasound scans of the heart to create the VR heart, found that surgeons preferred it for understanding the anatomy of their patient’s hearts.
The study, published in JTCVS Techniques, also reported that it increased their confidence and improved their decision making.
Two more types of scans have been added to the system – computed tomography (CT) and magnetic resonance imaging (MRI) – with the support of the BHF.
Every patient with congenital heart disease has their own set of unique changes to their heart.
It is hoped that by giving surgeons a better understanding of this and offering them an opportunity to practise and perfect operations, this technology will also help to improve the experiences of thousands of patients and their families each year.
Dr Sonya Babu-Narayan, associate medical director at the BHF and consultant cardiologist, said: “This new technology could help to make congenital heart disease surgery even more successful.
“It could also support people to better understand the heart or blood vessel abnormalities they are born with and what is being proposed to mend them, which can be empowering for people living with congenital heart disease.”