Dean Dunham 9pm - 10pm
4 September 2020, 01:13 | Updated: 4 September 2020, 01:19

There were more than 400 daily deaths involving Covid-19 at the peak of the UK's coronavirus outbreak, new analysis shows.
More than 3,000 deaths involving the virus occurred in one week in mid-April, according to the first UK-wide review of daily deaths by the Press Association news agency - who analysed data from Britain's statistics agencies to reveal the day-by-day death toll up to the end of July.
The number of coronavirus victims in care homes multiplied by five between the start of April (93 on the 1st) and the peak on the 17th, which claimed the lives of nearly 500 residents (490).
At this point, there was no testing of staff or residents in England, Scotland, Wales and Northern Ireland, whether people had symptoms or not.
Care home providers had also not been advised to restrict workers moving between facilities at this time.
Carl Heneghan, professor of evidence-based medicine at the University of Oxford, argues that the movement of staff between homes played a "huge" part in helping the virus spread while effective testing was not taking place.
Watch: 'She's not my mum anymore' - care home resident's daughter
Read more: Care Association Chair - lack of testing in care homes 'failure of system'

Johnson: We need a "proper investigation" into care homes deaths
From mid-March, thousands of hospital patients were discharged into care facilities while the acquisition of personal protective equipment (PPE) also came under strain.
The PA analysis comes ahead of the six-month anniversary of the first care home resident death involving Covid-19 on Sunday.
It found there were more than 400 deaths involving the disease in the UK on 11 different days in April.
The analysis also revealed there were 9,074 care home deaths across the UK by 26 April, when the first UK nation announced that providers should restrict staff movements.
This number represented 51% of the total fatalities up to 31 July.
Meanwhile, there were 9,776 care home deaths across the UK by 28 April, when the first UK nation announced testing for all care home staff, regardless of symptoms.
This number represented 55% of the total fatalities up to 31 July.
Watch: 'My mum's had enough, she wants to die' - caller tells James O'Brien
Read more: Government 'abandons' care home testing pledge
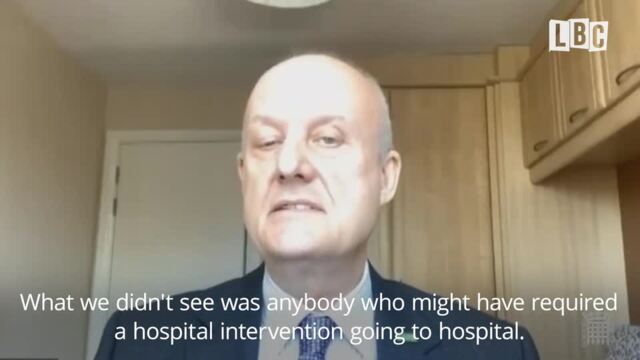
Care England CEO- We should've focused on care homes from start of pandemic
England's Chief Medical Officer Chris Whitty said in July "major risks" in social care settings were not considered early on, including staff working in multiple residences and those not paid sick leave.
Asymptomatic testing was first announced in England on 28 April, despite Public Health England (PHE) saying it was a concern from the end of March.
The first nation to advise care home providers to restrict staff movements between homes was Northern Ireland, on 26 April.
There was a gap of around two months between guidance from PHE advising care homes to share workforces in mid-March, to fresh advice to restrict staff movement announced on 13 May alongside funding to control infection spread in care homes in England.
Prof Heneghan said this was due to a lack of clinical experience in the government's advisory team and an absence of leadership.
Acknowledging care homes faced high levels of staff off-sick or self-isolating, he told PA: "The government should have advised that agency staff, if used, should be employed in a single care home and not travel between multiple care homes. That advice should have been given in the middle of March."
Watch: What's the truth on care homes? James O'Brien and Theo Usherwood investigate
Read more: Care home residents and staff 'to wait five weeks for Covid-19 tests'

Nick Ferrari grills Care Minister over failures in care homes
This should have been accompanied by funding to increase staffing levels, he added.
He believes this should be applied going into winter, but has seen no "sense of urgency" about protecting care homes.
Care England chief executive Professor Martin Green said guidance has been "slow to come to fruition" and addressing this, particularly with regards to visits, is a matter of urgency.
He said: "Many care homes locked down before national guidance came into force.
"Unfortunately patients were discharged from hospital without testing and this, compacted with insufficient PPE, created huge challenges for care homes.
"Routine testing is absolutely essential in order to establish confidence in the system for residents, staff, relatives and beyond."
The potential risks of staff movement were first discussed at a meeting of the Scientific Advisory Group for Emergencies (Sage) on 21 April.

Will the Government accept that it was too slow to act on care homes?
Dr Ian Hall co-authored the paper discussed, which was not made public until 19 June.
The University of Manchester academic told PA concerns around staff movement should have been made public as soon as possible and that, given capacity issues, he believes staff should have been prioritised for testing over symptomatic residents.
But he said: "What we weren't aware of at the time back in April and May was the complexity of the staffing situation, and so one of the concerns was, I know, 'if we go too hard on the potential for staff being a vehicle for transmission, then a lot of staff might be absent and that might affect the care needs of the otherwise healthy but vulnerable residents'.
"So it's a very delicate balancing act between trying to limit infection introduction and ensuring care is still provided."
UK care home provider MHA called for greater levels of investment in the sector, a better testing regime and "no slip-ups or delays", adding that the same mistakes cannot be made again.
Chief executive Sam Monaghan said: "What this analysis does is confirm that during the peak of the virus the sector, despite following all of the best infection control measures, were not supported with what turned out to be the additional critical tools we needed to manage the spread of the virus."

Heartbreaking call from care home resident's daughter
The senior national officer for Unison, Gavin Edwards, said social care must be considered an "essential public service" in the UK with pay and workforce conditions prioritised, to prevent a second wave occurring similar to the first.
He said: "Social care workers are often paid poverty wages, employed on zero-hours contracts and given no sick pay. In addition, many have faced a massive drop in income if they follow guidance and self-isolate. This clearly helped to drive infection rates in the sector."
A Department for Health and Social Care spokesman said: "We have been doing everything we can to ensure care home residents and staff are protected, including testing all residents and staff, provided 200 million items of PPE, ring-fenced £600 million to prevent infections in care homes and made a further £3.7 billion available to councils to address pressures caused by the pandemic - including in adult social care.
"As a result of actions taken, almost 60% of England's care homes have had no outbreak at all and the proportion of coronavirus deaths in care homes is lower in England than many other European countries."
Listen & subscribe: Global Player | Apple Podcasts | Google Podcasts | Spotify